Facial nerve neurinoma is a rare entity, although of great interest, especially from the point of view of the differential diagnosis of the causes of peripheral facial palsy.1 Neurinomas are benign tumors, derived from Schwann cells. They manifest mainly as peripheral facial palsy, which can be slow, gradually affecting several nerve branches, or with a sudden onset.1,2 They progressively invade the middle ear and the posterior wall of the external auditory canal, causing loss of auditory acuity.1,2
Facial nerve neurinoma has an incidence of 0.15–0.8%.2–4 Recent studies suggest that the most common anatomical location would be in the tympanic and vertical nerve pathway, but more recent studies have observed its presence in the geniculate ganglion.2,4
Advanced current radiological techniques, mainly high-resolution computed tomography (CT) and magnetic resonance imaging (MRI),3 have provided an earlier diagnosis. The advent of MRI had a significant impact on the diagnosis and management of neurinomas of the facial nerve, as in addition to the early diagnosis, there is greater accuracy regarding the limits and extent of lesions.3
In this report the aim was to report the occurrence of a facial neurinoma located near the geniculate ganglion, although it was unaffected.
Case presentationA male patient, 28 years old, reported labial deviation to the left since childhood, progressing in the last eight months to palsy in the upper third of the face, perceived during medical assessment. He has had hearing loss and intermittent tinnitus on the left for two years.
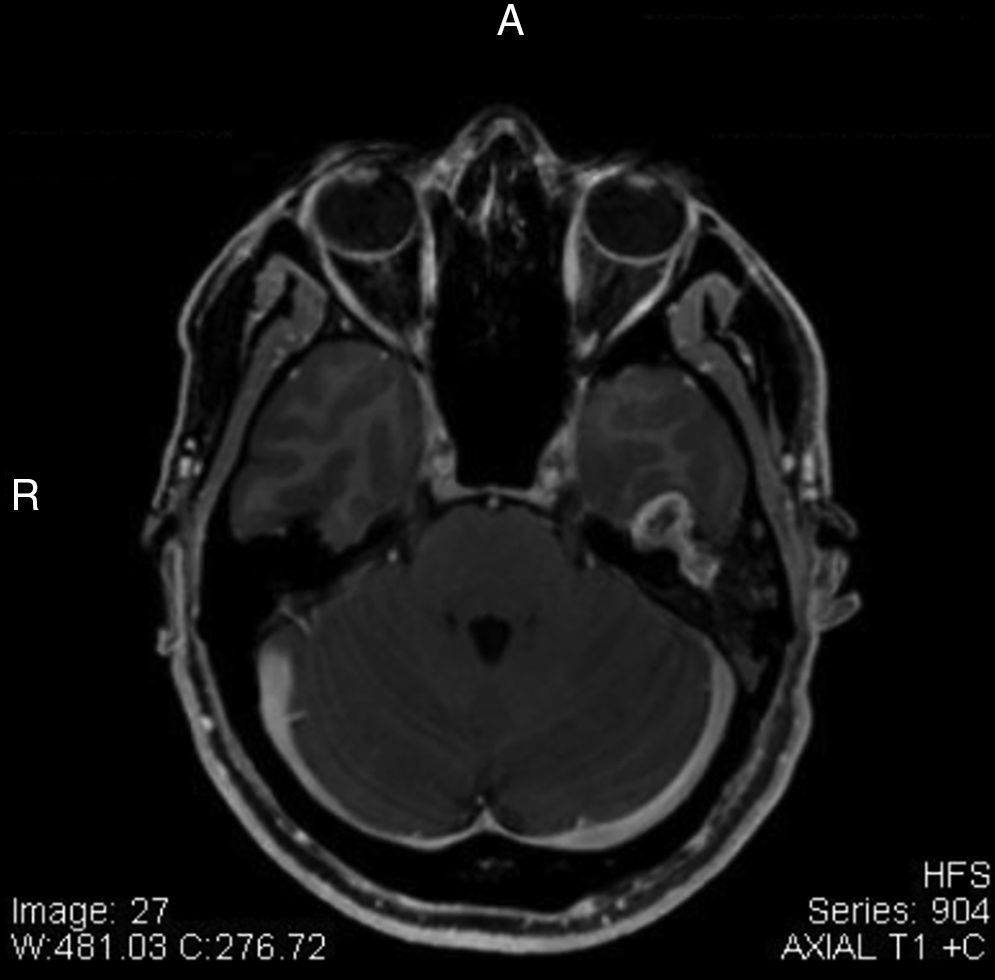
Otorhinolaryngological assessment showed Grade II House-Brackmann (HB) facial palsy to the left. MRI showed extensive formations in the topography of the left facial nerve canal near the geniculate ganglion, with hyposignal on T1 and hyperintense on T2, suggestive of facial nerve neurinoma. Treatment options were discussed with the patient, who decided to select clinical follow-up.
After two years of follow-up he developed worsening of peripheral facial palsy, HB grade IV, and the MRI showed increased volume of the lesion in comparison to the previous assessment, measuring 1.7×1.3cm (Fig. 1), compressing the lower temporal gyrus.
The choice of surgical approach was decided, considering the findings and neurosurgery team assessment.
Pure tone audiometry showed moderate conductive loss to the left and normal hearing to the right. Impedance audiometry resulted in curve type A, bilaterally. Electromyography was compatible with partial lesion of the left facial nerve, demonstrating severe intensity and signs of activity without fibrillation. CT scan of the temporal bones showed a mass in the tympanic region of the facial nerve, compressing the ossicles. Tegmen erosion was observed, with probable maintenance of dura mater.
The patient underwent surgery, which unveiled a lesion in the projection of the geniculate ganglion in the petrous portion of the temporal bone, with extradural extension that was soft, poorly vascularized, and extending to the mastoid facial canal. Presence of viable facial nerve near the stylomastoid foramen was observed. The lesion was resected and greater auricular nerve grafting was performed.
The patient persisted with Grade IV paralysis postoperatively. Histopathological examination disclosed the presence of cell schwannoma, with geniculate ganglion free of neoplastic involvement.
DiscussionThe management of facial neurinoma is a delicate process. Therapeutic options include clinical observation, surgical resection, and radiotherapy.4
Currently, surgical resection is reserved for patients with poor facial nerve function, House-Brackmann III, or worse. In patients with good function, HB I or II, clinical follow-up can be opted initially, combined with imaging follow-up.4 Radiation therapy is only indicated for patients with HB III or worse, with unfavorable clinical conditions for surgery.4
In this case, the authors initially observed good facial nerve function (HB II), and thus, clinical and imaging follow-up were initially chosen. Due to the progression of the lesion, both in volume size and clinical worsening of the facial nerve function (HB IV) during two years of follow-up, it was decided to perform surgical resection and greater auricular nerve grafting, with nerve function maintenance (HB IV).
Final commentsEarly surgical intervention is recommended in the following cases: intratemporal tumors extending to the parotid, tumors with multiple segments extending to the cerebellopontine angle and middle fossa, rapidly growing lesions, or those showing compression of the temporal lobe.4
Conflicts of interestThe authors declare no conflicts of interest.
Please cite this article as: Passos IM, Massuda ET, Hyppolito MA, Colli BO, Damico TA. Rare case of neurinoma of the facial nerve. Braz J Otorhinolaryngol. 2015;81:226–7.
Institution: Hospital das Clínicas da Faculdade de Medicina de Ribeirão Preto, Universidade de São Paulo (USP), Ribeirão Preto, SP, Brazil.