Craniofacial osteomas are rare conditions, and few cases have been described in the literature.1,2 They are benign tumors of bone characterized by cortical or medullary bone proliferation, affecting mainly young adults.2,3 Peripheral osteomas have been described in the frontal and ethmoid bones and the maxillary sinus, but they are unusual in the mandible.3,4 In the mandible, the most frequent locations are the angle and the condyle, followed by the mandibular body and the ascending ramus.4
This is a case report of an exuberant osteoma of the internal aspect of the left angle of the mandible in a surgically treated asymptomatic patient.
Case reportA 41-year-old female resident of São Paulo, Brazil, presented to the outpatient clinic with the complaint of a hard, slowly growing, painless swelling in the left submandibular region for approximately one year. She had experienced no weight loss, dysphagia, and dyspnea, had no smoking or drinking history.
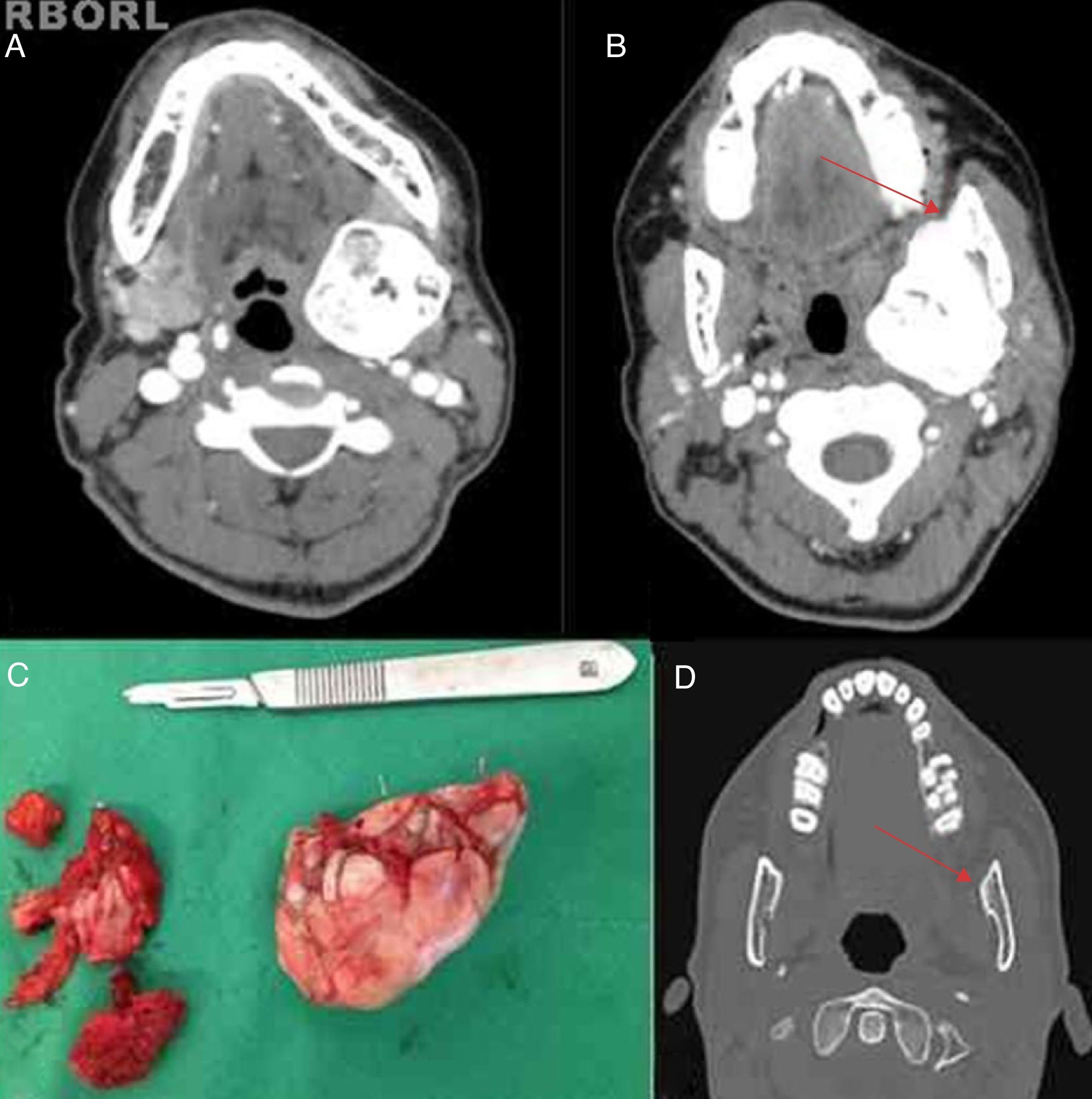
On physical examination, she was in good health and was eutrophic (BMI: 24.6). Oroscopy, otoscopy, and rhinoscopy revealed no abnormalities. Two nodules could be palpated in the neck; they were hard and fixed to deep tissue planes. A 3-cm nodule was found at level II; another 2-cm nodule was found on the left angle of the mandible. Computed tomography indicated that the latter bony lesion was single, lobulated, and pedunculated on the left inner face of the mandibular angle (Fig. 1A and B).
(A) Contrasted computed tomography of the face, showing an osteoma of the mandible. Axial view exhibiting large mass with a bony component occupying the parapharyngeal space. (B) Computed tomography, axial view exhibiting pedicle (red arrow) on the internal aspect of the left angle of the mandible. (C) Surgical specimen, osteoma removed through resection of its pedicle to the left angle of the mandible. (D) Follow-up computed tomography demonstrating no lesions (the red arrow shows the point at which the osteoma was pedunculated).
Total resection via cross-sectional cervicotomy ipsilateral to the lesion was performed through osteotomy of the lesion pedicle (Fig. 1C). The final histopathological study of the specimen revealed an osteoma. The patient had a good postoperative course and has been followed up as an outpatient for four months. She is asymptomatic and has no signs of recurrence (Fig. 1D).
DiscussionMost osteomas consist of small lesions; however, larger lesions can occur, as in this patient's case. Even though they can affect individuals at any age between 16 and 74 years,1 these tumors are more often found in patients aged 20–50 years.5 A number of studies report no difference between genders,2 whereas others indicate a female predominance.4 The current case is in line with the literature regarding age and gender.
As in our case, patients with osteoma are usually asymptomatic and the lesion grows slowly. When the mandible is affected, they may show changes in bite and dentition.2 Osteomas can be sessile or pedunculated,2,6 and are found in the mandible angle, condyle, or molar body regions.2 In the present patient, the lesion was pedunculated to the left mandible angle and had a cranial growth.
Diagnostic work-up can be complemented with a plain radiograph, a panoramic radiograph, or computed tomography; tomography is considered best for delimiting size, location, and anatomical relationships with adjacent structures.1
Final commentsSurgical management should be indicated both for cosmetic complaints and for diagnostic confirmation, especially in bulky lesions. Differential diagnoses include inflammatory or neoplastic diseases, such as ossifying fibroma, exostosis, chronic osteomyelitis, chondroma, osteosarcoma, Paget's disease, fibrous dysplasia, and osteoblastoma.1,6 On the basis of the clinical presentation and imaging studies, resection of the lesion via cervicotomy was chosen; mandibular reconstruction was not needed.
Conflicts of interestThe authors declare no conflicts of interest.
Please cite this article as: de Souza PD, Leonhardt FD, Ahumada NG, Abrahão M, Cervantes O. Giant osteoma of the mandible. Braz J Otorhinolaryngol. 2015;81:107–8.